
TMS


WHAT IT ISA Non-Medication Path to Change
Sometimes depression or anxiety persists even with thoughtful treatment. That can feel discouraging, especially when you’re doing the work and still not getting relief.
Transcranial Magnetic Stimulation (TMS) is a noninvasive, evidence-based treatment that supports the brain directly. Using focused magnetic pulses, TMS stimulates networks involved in mood, motivation, attention, and emotional regulation — without medication, anesthesia, or sedation. Most people remain fully awake during sessions, drive themselves home afterward, and return to their normal daily activities.
At MBLDN, TMS is provided using a Magstim system with FDA-cleared indications for depression, OCD, and anxious depression.
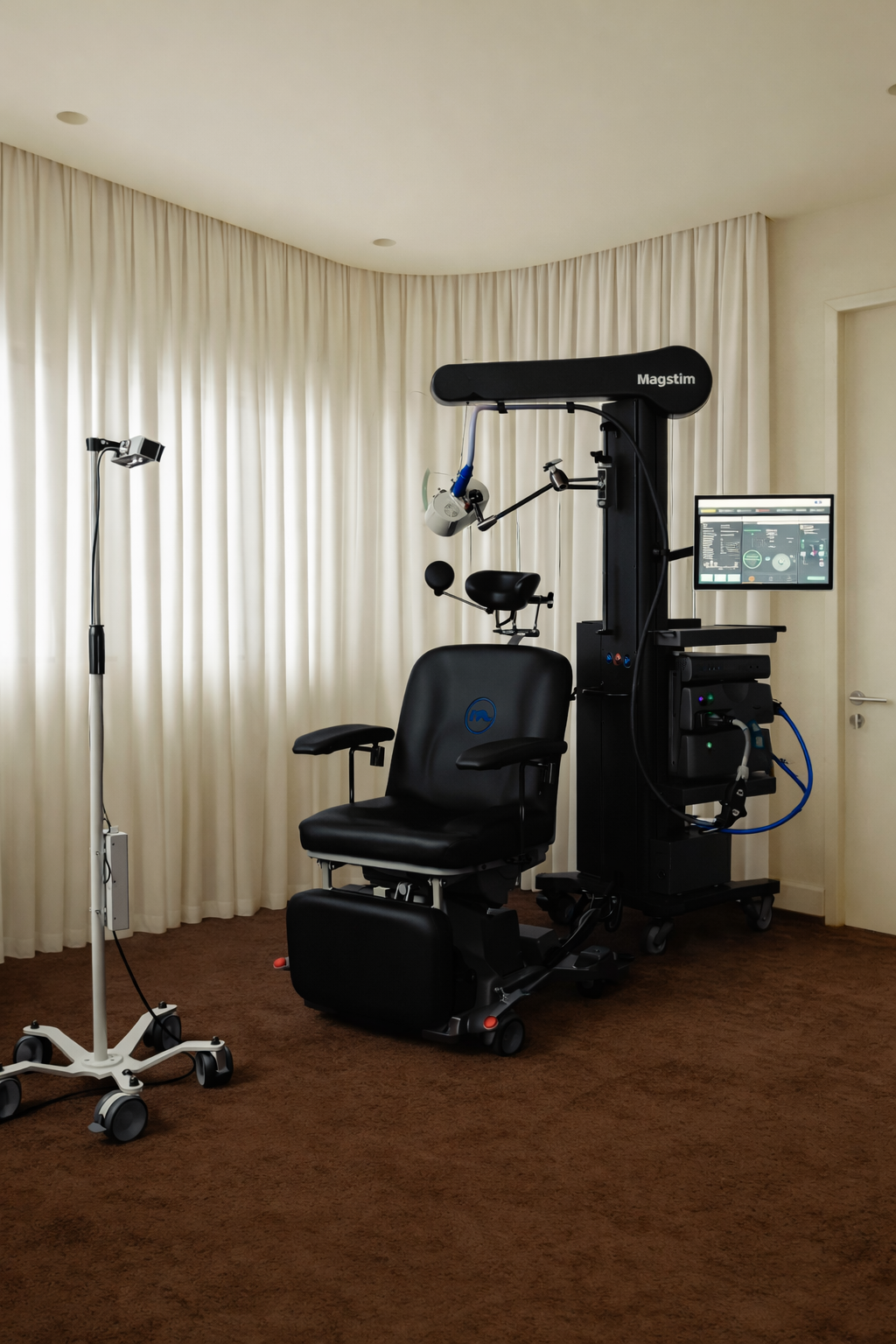

HOW IT WORKSA Gentle Way to Support Brain Circuits
TMS works by gently stimulating specific brain regions involved in regulation — particularly areas connected to mood, attention, planning, and emotional flexibility.
Repeated sessions help the brain retrain these networks over time. The goal isn’t to change who you are. It’s to strengthen the circuitry that allows you to respond with more resilience, clarity, and engagement with life.
Many people experience improvement gradually — not as a sudden shift, but as a return of capacity: better focus, more energy, improved sleep, and increased motivation.

WHO IT MAY BE FORA Treatment for Persistent Depression
TMS may be a meaningful option for individuals experiencing depression that has not improved enough with traditional treatments, or for those who prefer a non-medication approach that works directly with brain networks involved in mood and regulation. It is most often considered when antidepressant medications and therapy have provided only partial relief or have been difficult to tolerate.
TMS is FDA-cleared for major depressive disorder, obsessive-compulsive disorder (OCD), and for reducing anxiety symptoms in individuals with depression.
The best way to determine whether TMS is appropriate is through a careful evaluation of your history, current symptoms, prior treatments, and treatment goals.
You may be a good candidate if you:
Have major depressive disorder that has been difficult to treat
Have tried one or more antidepressant medications without adequate improvement
Experienced side effects from medications that limited their use
Are experiencing persistent symptoms such as low mood, low motivation, fatigue, or difficulty concentrating
Prefer a non-invasive treatment option that does not require daily medication
Are able to attend regular in-office sessions over several weeks
PROCESSTMS is delivered as an individualized course of treatment, similar in spirit to physical therapy for the brain.
Most treatment plans include:
Sessions lasting about 9–20 minutes
3–5 visits per week
A course lasting about 4–6 weeks
A gradual taper afterward when appropriate
Before treatment begins, we complete a careful setup appointment to determine precise placement and individualized intensity so treatment is both effective and comfortable.
There are different evidence-based protocol styles, including standard rTMS and shorter theta burst approaches, which have shown comparable effectiveness.
INFORMATIONTMS is one of the most strongly evidence-supported non-medication treatments for depression.
Effectiveness
Research and clinical experience show:
Response rates (about 50% improvement): 45–60%
Remission rates: 30–40%
If symptoms return later, some individuals benefit from booster sessions or a repeat course.
Safety
The most serious potential risk is seizure, but this is very rare when appropriate screening and safety protocols are followed. We monitor your response throughout treatment to keep care both effective and comfortable.

Side Effects
TMS is generally well tolerated. Common side effects include mild scalp discomfort, headache, facial muscle twitching during pulses, and lightheadedness. These typically improve as treatment continues.



COVERAGECare that is Careful, Individualized, & Grounded
TMS is often covered by insurance when medical criteria are met, though most plans require prior authorization and benefits vary by policy. MBLDN Psychiatry & Wellness is in network with Aetna, Anthem Blue Cross, Cigna, Optum / UnitedHealthcare, Blue Shield of California. If you’re considering TMS, our office can help you understand your benefits and navigate the approval process.
FREQUENT QUESTIONSConsidering TMS can bring curiosity, hope, and uncertainty.
These answers offer a clearer picture of what treatment involves so you can decide what feels right for you.
-
During treatment, you remain awake and alert. The device makes a clicking sound, and most people feel a tapping or pulsing sensation on the scalp where the stimulation is delivered. You may notice mild muscle twitching in the forehead or jaw during certain pulses. The first few sessions can feel unfamiliar, but most people adjust quickly as treatment becomes routine.
-
Some people experience mild scalp discomfort or tenderness, especially during the first few sessions. This usually improves as your body acclimates. We can adjust positioning, intensity, and comfort measures to make the experience more tolerable while maintaining effectiveness.
-
TMS works gradually. Some people begin noticing subtle shifts within the first couple of weeks, while others experience changes later in the treatment course. Improvement often feels like a gradual return of capacity — more energy, clearer thinking, improved sleep, or increased motivation — rather than a sudden change.
-
Yes. TMS does not require anesthesia or sedation, and most people drive themselves to and from sessions and continue their normal daily activities afterward.
-
In many cases, yes. TMS is often used alongside medications or therapy. We’ll review your current treatment plan together to ensure everything is safe and coordinated.
-
TMS has been studied extensively and is considered safe when appropriate screening and protocols are followed. The most serious potential risk is seizure, but this is very rare. We minimize risk through careful evaluation, individualized treatment settings, and ongoing monitoring throughout your course.
-
The most common side effects include:
Scalp discomfort or tenderness
Headache
Facial muscle twitching during treatment
Lightheadedness
These effects are usually mild to moderate and often improve over time. If anything feels uncomfortable, we adjust the treatment to support tolerability.
-
TMS is often covered by insurance when medical criteria are met, though most plans require prior authorization. Coverage varies based on your specific policy. Our office can help you understand your benefits and guide you through the approval process.
LET'S GET STARTEDCare Begins with a Conversation
Through an initial consultation, we explore your history, symptoms, and goals to determine the most appropriate integrative or interventional treatment approach for you.

